Specialities
Joint, Knee, Hip Replacement Surgery in Chennai
A joint is where the ends of two or more bones meet. For example, a bone of the lower leg, called the shin or tibia and the thighbone, called the femur, meet to form the knee joint or hinge joint. Likewise, the hip is a ball and socket joint. It is formed by the upper end of the thighbone-the ball at the end of the femur, fitting into the socket-part of the pelvis called the acetabulum. Other joints in the musculoskeletal system are at the shoulder, ankle, elbow, and wrists. The ends of the bones are covered in cartilage, which help to cushion and enable smooth, easy movement. When the cartilage wears away either due to injury or because it is diseased, the bones become rough and grind against each other, causing disability and pain.
Why does pain develop in joints?
With age, the cartilage tissue that cushions our bones become thin. As a result, the bones start rubbing against each other or pressing against nerves and surrounding tissues. This causes joint pain. Falls and injuries in the past, osteoarthritis, osteoporosis, sedentary lifestyle, lifestyle habits and medications for certain conditions all increase the risk for joint pain. Further, pain in the knee joint can trigger pain in the hip joint and vice-versa.
Several types of conditions can cause joint pain or cause disability, consequently requiring a patient to consider joint replacement surgery. A joint replacement surgery would be suggested when non-surgical treatments like medications, physiotherapy and changes to a patient’s daily activities fail to provide any relief from pain and disability. Anti-inflammatory medications are prescribed to treat a patient non-surgically, along with physiotherapy and individually designed exercises that can be performed at home.
How will I know if joint replacement surgery is required?
A qualified orthopedic doctor will assess the extent of your pain. He/she will then put you on other courses of treatment such as physical therapy and medication. When none of these work, and the pain becomes severe, accompanied by swelling and redness in the joints, or extreme difficulty in moving, bending or straightening up, it may be time for joint-replacement.
When a patient is referred for a joint replacement program, the Orthopaedic Surgeon will suggest treatments based on the findings and diagnosis, taking into consideration the age, activity levels and medical history of the patient. The evaluations will be based on radiological, medical, physical and historical records of the patient. Both non-surgical and surgical options will be considered and discussed by the orthopaedic surgeon, as a part of counselling and educating the patient.
Total joint replacement is considered when non-surgical efforts fail to provide any modicum of relief from pain. Joint replacement is a surgical procedure in which arthritic or damaged joints parts are removed and replaced with plastic, metal or ceramic prosthesis or devices which are designed to duplicate movement of the joint, as closely as the original joint.
Is this an inpatient or outpatient surgery?
The patient must stay in the hospital for 1 or 2 days so it’s an inpatient procedure. Physical therapy and medication will begin almost immediately and will continue even after you he/she is discharged. There will be clear instructions on activity and lifestyle which must be followed for a good outcome.
Once you have chosen to have your joint replaced, the orthopaedic surgeon will schedule the surgical procedure. The surgical team will administer anaesthesia, which could be either spinal or general. Once the anaesthesia takes effect, the surgical team will replace the damaged joint with a prosthesis.
The length of the surgery will depend on the extent of damage to the joint and therefore, each surgery will be different, depending on whether there are other complications involved. Post-surgery, the patient will be held in a recovery room, until such time the anaesthetic effect has worn off.
What is the success rate for such surgeries?
Hip-joint and knee-joint replacement surgeries have been around for long. The success rate is as much as 95%. People who have undergone joint-replacement can enjoy reduced pain, reduced discomfort, increased mobility and improved quality of life after surgery. There are various dos and don’ts after the surgery and the doctor will educate you on the same thoroughly
After a knee or hip replacement surgery, the process to help you regain your mobility will begin, such as standing or walking. To begin with, our trained and experienced physiotherapists will assist you in strengthening the muscles with gentle exercises, so that you can regain mobility. If the joint replacement was in your shoulder, generally you will be encouraged to begin exercising it the very same day of the surgery.
Types of Joint Replacement Surgeries
Many of the joints in the body can be replaced with artificial joints that allow the patient to regain a full range of motion and engage in everyday activities. Common joint replacement surgeries include:
- Hip replacement
- Knee replacement
- Shoulder joint replacement
- Elbow replacement
- Wrist joint replacement
When is Joint Replacement Recommended?
Some medical conditions and injuries can lead to severe joint pain and loss of flexibility/mobility. Among the common reasons for this are:
- Degenerative diseases like osteoarthritis
- Fractures that cannot/do not heal properly
- Various medical reasons, including lifestyle issues
The preliminary course of treatment is usually through medication, physical therapy, and exercise. If this is ineffective or if the patient’s condition is such that immediate amelioration is essential, joint replacement may be advised.
How is the Need for Joint Surgery Diagnosed?
Joint pain may have many causes, some of which may not require surgery. An orthopaedic specialist will make a careful diagnosis to ensure that joint replacement can cure the problem. In most cases, a diagnosis that points to the need for joint replacement surgery can be made through a physical examination of the joint, a study of the patient’s medical history, and the use of x-ray and scans.
Preparing for Surgery
If the surgical procedure is an elective, there will be time for you and your doctor to prepare. In the lead-up to the process, you will be required to undergo various tests and examinations to ascertain your overall health status and spot any issues that may affect the surgery or require any modification in the procedure. If needed, pre-surgical medication may be prescribed to prepare your body for the surgery.
There is also much that you can do to prepare for the joint replacement. Ask your doctor about an exercise routine and diet that will help get your body ready for the surgery. After you return from the hospital, your mobility will be limited for some time. Make advance arrangements for:
- A caregiver to be available
- Food to be prepared
- Removing any unnecessary objects in the home that could impede your movements or cause you to place stress on the new joint. Your actions will be restricted, even around the house, for some time, and rest is an essential part of the recovery process. Make advance arrangements to be as comfortable and stress-free as possible.
Surgical Procedure
The exact nature of the procedure will depend on the joint that is being replaced. In general, the procedure is done under general anesthesia. The surgery takes a few hours, during which an incision is made, the damaged cartilage and bone are removed, and a prosthetic joint is fixed in place. This joint, which may be made of metal, plastic, or ceramic material (the doctor will decide which is suitable for you), will mimic the removed natural joint’s shape and movement.
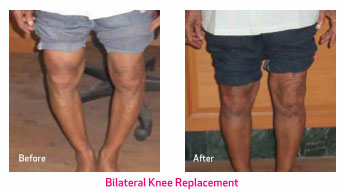
After the procedure, you will be required to stay in the hospital for a few days. The duration will depend on the type of joint replacement is done and whether more than one joint was replaced. For example, if it was a bilateral knee replacement (both knee joints replaced), it may take you a little longer to be able to walk with the help of a crutch or cane.
Are there any risks from a joint replacement surgery?
All surgical procedures come with certain risk. The risk from joint-replacement surgeries include blood clots and infection. However, these are not very common. Further, since the doctors are aware of this, they will take necessary measure to minimize or manage the risk. Joint replacement surgery, while being commonplace, is a major procedure, and as such, there is always going to be some risk of complications. If they do occur, most complications can be treated quickly and have little impact on the recovery process. Your doctor will explain the possible complications to you while briefing you about the procedure. The common post-surgical complications include infection, nerve injury, development of blood clots, and problems with the prosthesis.
There are 2 types of possible complications that arise immediately after the surgery and those that may occur after some time. Your doctor will tell you about the potential long-term issues so you can identify any that may arise and get treatment without delay.
Recovery
Recovery and rehabilitation are different for each person. Typically your doctor will encourage you to start using your new joint shortly after the operation. This may be difficult at first, but the difficulty will reduce with regular use. You must follow the doctor’s instructions on exercise, rest, diet, etc. You may be prescribed pain reduction medication and food supplements to help you regain your strength.
is an important part of recovery, and you will be given exercises to help restore movement and flexibility of the joint. Physiotherapy may also be prescribed during the recovery period.
In the case of knee or hip joint replacement, you will have to use a crutch or cane to support yourself in the early stages of recovery. The need for this will gradually reduce until you can walk normally without support.
Preventing Joint Problems
Preventing joint problems is a matter of common sense and practical care. While each person’s physical care needs are different, in general, these tips will help to keep joints healthy:
- Get enough exercise. The more you move, the less stiffness of the joints you will experience.
- Do not spend long hours sitting in the same position, whether working, watching TV, or something else. Take a break every hour or so, and walk around for a few minutes.
- If your preferred form of exercise carries some risk of impact injury, wear protective equipment like knee and elbow guards.
- Low-impact exercises like walking, swimming, cycling, etc., place the least stress on the joints.
- Before starting your exercise, do some light warm-up movements to loosen up the joints, ligaments, and tendons, so they do not have sudden stress placed on them.
- Know your physical limitations and do not try to exceed them. Tiredness after exercising is normal, but pain, especially pain that stays for some time, is not. If your exercise regimen causes any discomfort, change it.
- Control your weight. The more you weigh, the more load on your joints. If you are even slightly overweight, you are placing more stress on your joints. As a rule of thumb, every 1 kg reduction in body weight results in a 2 kg reduction of pressure on your knee or hip joints.
- Your diet plays an important role in joint health. Ask your doctor or consult a nutritionist about the right diet for you.
- Ensure you maintain the right posture, especially when sitting down or walking.
- Avoid taking supplements or going in for non-specialist treatment for joint pain. These could make the problem worse. Consult your doctor before trying anything.
- Finally, consult an orthopedic specialist without delay if you have joint pain or suffer a possible injury.
